Introduction
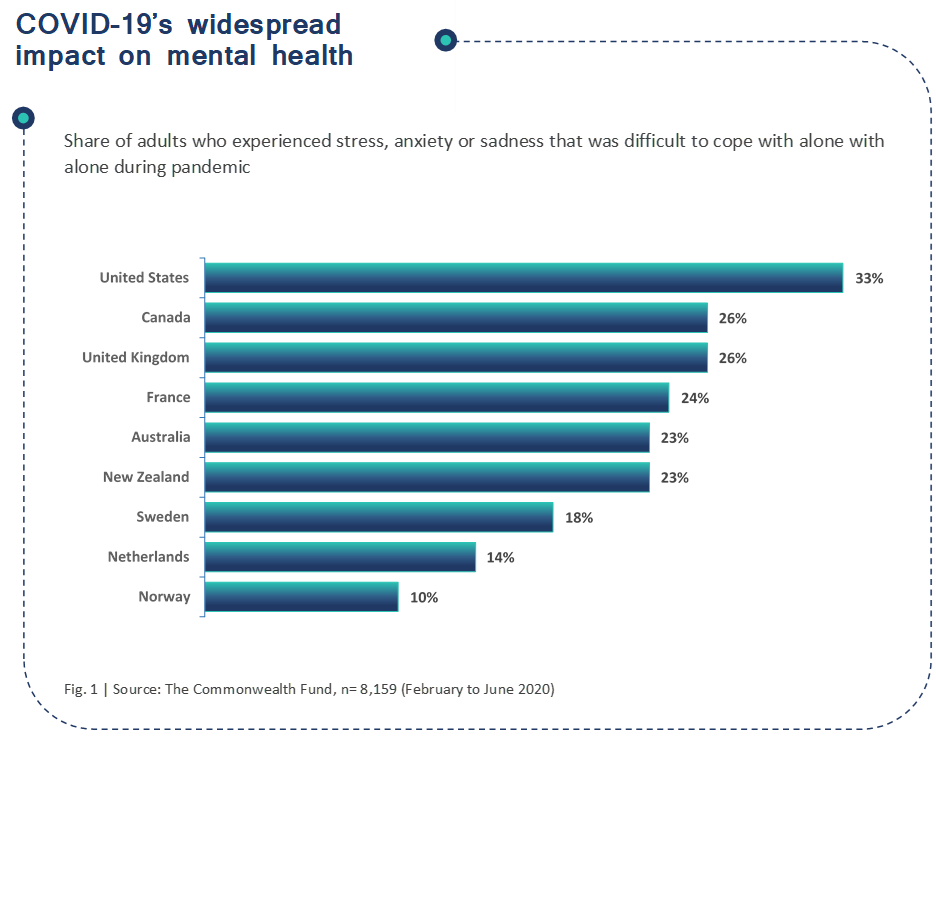
We live in turbulent times impacted by the COVID-19 pandemic, and hence the issue of mental health is not only relevant but crucial. Mental health is more than the presence or absence of a mental illness. It is a crossroad between emotional, psychological, and physical well-being. The pandemic and the ensuing economic downturn have had a significant impact on many people’s mental health and created new hurdles for those who already have mental health issues (Figure 1). Along with the health impacts of the disease, the pandemic has led to, self and social isolation, disconnection from family and friends, quarantine, and lockdowns on movement resulting in more people than ever experiencing feelings of helplessness, isolation, grief, anxiety, and depression. Consequently, demand for health support services has increased exponentially.
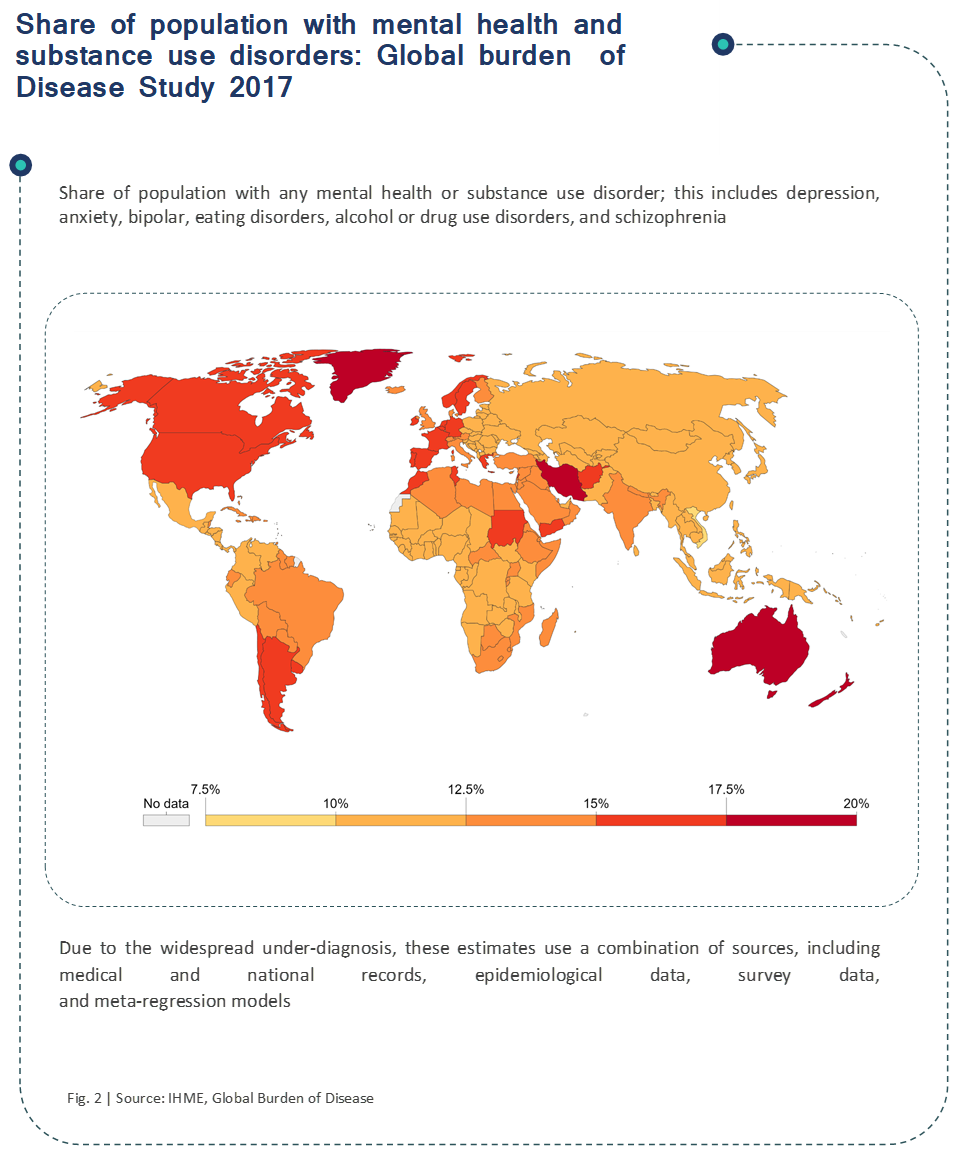
The global situation of mental health even before the pandemic was alarming. In 2017 it was estimated that 792 million people were affected with mental health disorders, that translated to one in ten people globally. Figure 2 shows the share of the population with mental health and substance use disorders in 2017. There were 1 in 5 people in the deep red zones that are with mental health or substance use disorder. The ratio is deteriorating further during the pandemic.
During the pandemic, demand for mental health services outstripped availability, presenting opportunities for digital technology solutions to fill this emerging void while demonstrating capabilities to improve their efficacy and performance. This triggered progress and brought mental health to the forefront of the digital health revolution. This is reflected in the rapid adoption of digital media by formal mental health services, as well as the increase in demand as many countries prepare for a mental health pandemic.
Innovative mental health vendors are increasingly integrating digital technologies and virtual care to build a robust environment for end-to-end patient care, including guiding patients to in-person care when necessary. Because of these advantages, the majority of employer-sponsored insurance plans also have interactive and digital mental health treatment options. This set of tools offers scalable solutions and improved flexibility to the mental health care system, while also improving customer access and convenience.
We at Healthark Insights have been fortunate to work on various mental health programs with our clients and have had a chance to engage with a handful of major players as well as start-ups and innovators along the way. We have gained a deeper understanding of this mental health landscape and first-hand appreciation for the challenges facing the sector.
In the following sections, we share our learnings regarding the digital mental health sector, including key opportunity areas, the competitive landscape, unmet needs, and consumer preferences, as well as challenges encountered while developing and implementing digital health solutions for mitigating mental health issues.
Mental Health Issues as a Result of COVID-19 Pandemic
Outbreaks can have a profound and broad spectrum of psychological impacts on people. At an individual level, new psychiatric symptoms in people without mental illness can precipitate, or aggravate the condition of those with pre-existing mental illness and cause distress to the caregivers of affected persons. Individuals may experience fear and anxiety of falling sick or dying, helplessness, or blame of other people who are ill, potentially triggering off a mental breakdown, regardless of their exposure. Many people have lost their jobs or are working reduced hours. Due to the enormity of this pandemic and the global shut down the sense of normality has been turned upside down. The uncertainty over what even the near future holds will make sustained attention a challenge.
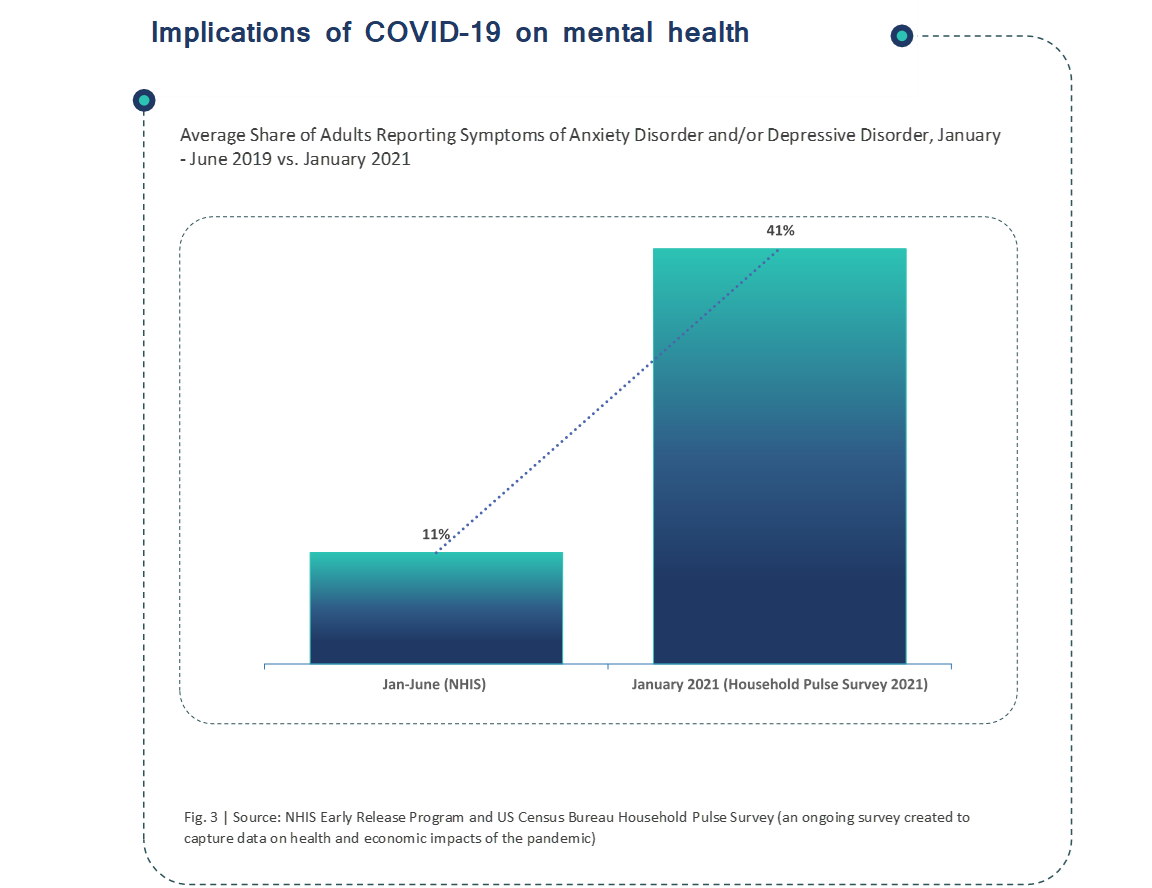
The COVID-19 pandemic and the resulting economic recession have negatively affected many people’s mental health and created new barriers for people already suffering from mental illness and substance use disorders. During the pandemic, about 4 in 10 adults in the US have reported symptoms of anxiety or depressive disorder, a share that has been largely consistent, up from one in ten adults who reported these symptoms from January to June 2019 (Figure 3). A KFF Health Tracking Poll from July 2020 also found that many adults are reporting specific negative impacts on their mental health and well-being, such as difficulty sleeping (36%) or eating (32%), increases in alcohol consumption or substance use (12%), and worsening chronic conditions (12%), due to worry and stress over the coronavirus. As the pandemic wears on, ongoing and necessary public health measures expose many people to experiencing situations linked to poor mental health outcomes, such as isolation and job loss.
Significant psychiatric conditions could be found varying from depression, anxiety, panic attacks, somatic symptoms, and post-traumatic stress disorder symptoms, to delirium, psychosis, and even suicidality, which could be associated with younger age and increased self-blame. Some individuals have health conditions that make them anxious (and vulnerable) about catching the virus. For persons grieving from the traumatic and sudden loss of loved ones from the outbreak, the inability to gain closure can result in additional stresses, anger, and resentment.
At the community level, there could be distrust towards other individuals in terms of disease spread and the government and healthcare services in terms of their capability to manage the outbreak. With the closure of community services and the collapse of industries negatively impacting the economy, a lot of people face financial losses and risk unemployment, which will be intensifying the negative emotions experienced by individuals.
Internationally, stigma and blame targeted at communities affected by the outbreak by other countries due to a fear of infection impede cross-national trade. All these emotions can be amplified by pre-existing depressive and anxiety disorders, contributing to the increased rumination of contracting the disease, and this can profoundly remodel people’s behavior and social interaction with others. Psychological responses could affect a person’s particular health-seeking behavior. Feelings of helplessness and anxiety can motivate some people to use unproven methods and remedies that may have detrimental effects.
Opportunities and Growing Landscape of Digital Mental Health Solutions
The opportunity for a digital change of mental health is one of the biggest in all of healthcare. This is partly because most mental health services are limited to verbal exchanges that can easily be provided over the internet. More specifically, “all nations are developing countries,” as The Lancet Commission on Global Mental Health and Sustainable Development puts it. That is, in high-, middle-and low-income countries, the distance between what people need and what current structures can offer is currently so wide that only a technological transformation in access, efficiency, and participation can meaningfully close it. Digital mental health resources are no longer a potential luxury for modern health systems; they are a pressing need. In a significant number of resource-poor and low- and middle-income countries, using digital technologies to provide mental health care could potentially serve as a viable adjunct or alternative to conventional services in closing the mental health gap.
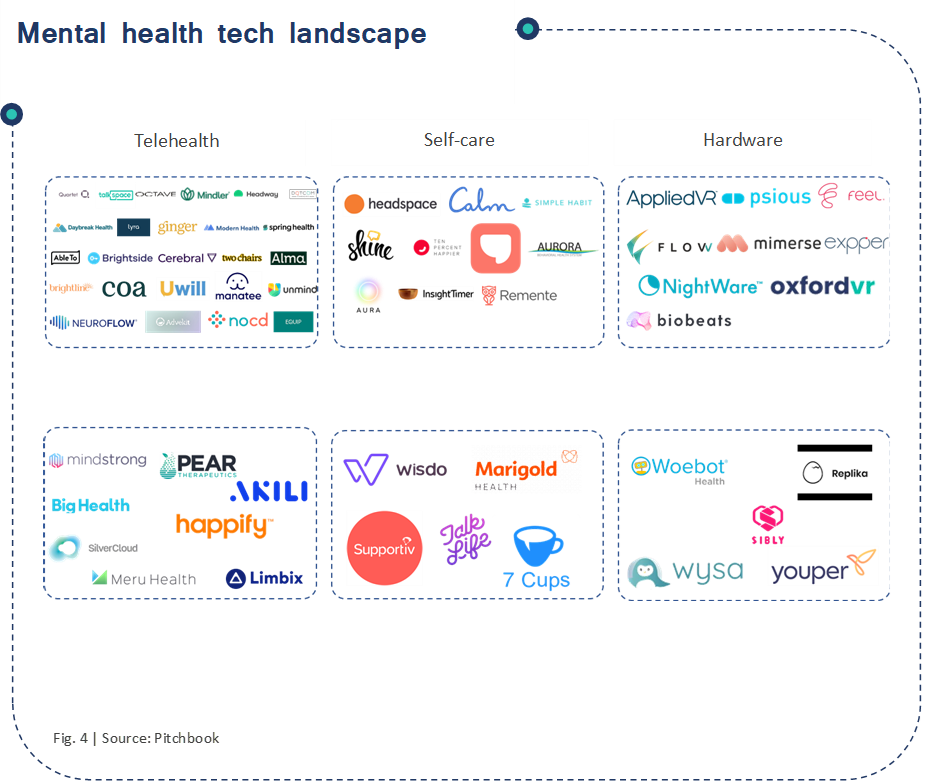
In recent years, new digital tools for mental health assessment, support, prevention, and treatment have exploded in popularity. According to a report by the WISH 2020 Forum on Mental Health and Digital Technologies, there are over 10,000 mental health apps available in the market today, and around 100 new mental health start-ups are launched each year. However, many of these apps and start-ups underperform. Figure 4 depicts the rapid expansion of mental health start-ups; it is not comprehensive and depicts the most well-funded or promising companies.
Instant crisis text messaging, digitized or ‘gamified’ forms of cognitive-behavioral treatment (CBT), and online training packages for frontline staff are examples of products that have proven effectiveness, are low cost, and are already assisting millions of people around the world. However, many other tools have underperformed, meaning the gap in ‘effective coverage’ for mental health disorders remains, with as few as one in 10 people in need benefiting from traditional mental health services – even in well-funded health systems.
Mapping the unmet needs for better healthcare
The goal of using digital tools in mental health isn’t just to increase the scale and efficiency of current service models. The goal cannot be to provide services that are comparable to face-to-face care but are less expensive. Instead, digital innovation is required at every stage of the system, including rethinking and redesigning what is supplied, how it is delivered, who it is for, and how we know whether it works.
To execute any strategy in the mental health space, the foremost thing to be conquered is to establish a thorough understanding of the key need gaps and behavioral trends of the target audience, which would then ultimately translate into potential features for a minimal viable product. The objective is to develop a holistic view of the needs, behaviors, accessibility, utility of the digital platform.
Building Solutions: Determining Product Offerings
Once the key need gaps and desired features of any digital mental health initiative are established, we then move towards solution designing of the digital platform. An evidence-based approach works the best. The stakes are enormous for both patients and customers. If someone seeks therapy and has a negative experience with a digital mental health tool, it is a missed opportunity that could result in care being delayed.
According to the European Connected Health Alliance, there are over 380,000 health apps available for Apple and Android operating systems, with roughly 20,000 of them addressing mental health. However, with thousands of digital mental health solutions on the market, many companies aren’t doing enough to validate their solutions.
Developing an effective digital mental health solution that benefits users requires a careful approach to identifying the product’s specialization i.e., key or primary product offerings that will directly address the target audience’s needs along with ancillary services that can augment achieving the objective of the digital mental health program.
In our experience, sometimes, the primary offerings are not as enthusiastically received by the consumer as anticipated with the ancillary product offering garnering more traction. Hence, when it comes to solution designing being flexible with the product offerings would be a wise thought as they are prone to consumer perception and uptake which are unpredictable in nature.
Cognitive-behavioral and acceptance and commitment therapies, mood training programs, gamification, customizable settings, and forums are just a few of the tools and strategies that may be used to personalize mental health apps to suit the needs of users.
Implementation of a Digital Platform and Adoption Barriers
The roll-out and adoption of digital solutions is a lengthy and intricate process that frequently involves multiple stakeholders from many disciplines, a variety of decision-making procedures, and a series of personal or organizational value judgments. At an institutional level, the digital platform is subjected to evaluation around potential outcomes by the key stakeholders involved. This is followed by a complicated course of approvals across the management level due to which the objective of early intervention is not attained. When it comes to user acceptance, stigma and the fear of confidentiality breaches are the most commonly encountered roadblocks.
Another major challenge is the digital divide that exists between socioeconomic levels. Individuals in need of mental health services from lower socioeconomic backgrounds frequently have limited access to digital technologies, particularly those equipped with the apps that online mental health services rely on. Some of the barriers to the adoption of digital health initiatives basis our experience are highlighted below: –
A. Technology adoption
– Attitude towards technology
– Digital literacy
– Fitting with routine or lifestyle (paucity of time owing to long working hours)
– Competition from already existing digital health tools in the market
– Fear of discrimination & stigma
– Reliance on internet availability
B. Perceived utility
– Doubts about tool effectiveness both at an organization level and at a
user level
– Concerns over value-add over existing initiatives
C. Confidentiality concerns
– Passive data collection
– Privacy & security concerns
D. Language barriers
– The content and mental health counseling services on the digital health platform have to be made available in vernacular languages to ensure
Conclusion
The use of technology for mental health has come a long way in a few years. Past successes have shown us what is possible, but the gaps in our knowledge and approaches have also been revealed. We have hit a bump in the road, which allows us to take stock of our achievements and failures and to reconceptualize the needs and direction of this field of research. The ultimate success of the mental health technology revolution requires improving awareness, resolving stigma, strengthening implementation and accelerating innovation by challenging traditional ways of thinking.
The pandemic has put a spotlight on the value of digital and virtual mental health care, and by doing so might have thrown a lifeline to our mental health system. If we can harness learnings from the pandemic to drive increased, appropriate use of digital tools and virtual care, we can significantly improve the long-standing problems of inadequate access to mental health services.
Authors

Healthark insights

Healthark insights
Sources
- Digital Mental Health Challenges and the Horizon Ahead for Solutions
- The Digital Mental Health Revolution | Wish Forum Report 2020
- Barriers to and Facilitators of Engagement With mHealth Technology for Remote Measurement and Management of Depression: Qualitative Analysis
- Digital Mental Health and COVID-19: Using Technology Today to Accelerate the Curve on Access and Quality Tomorrow
- The digital mental health revolution: Opportunities and risks
- Digital Tools Are Revolutionizing Mental Health Care in the U.S.
- Global Burden of Disease 2019 report
- Global prevalence of mental health issues among the general population during the coronavirus disease-2019 pandemic: a systematic review and meta-analysis
- Mental Health Is a Growing Concern for Many During the COVID-19 Pandemic
- Mental Health Disorder Statistics: John Hopkins Medicine blog
Kindly fill in the following details. The report will be mailed to you.


